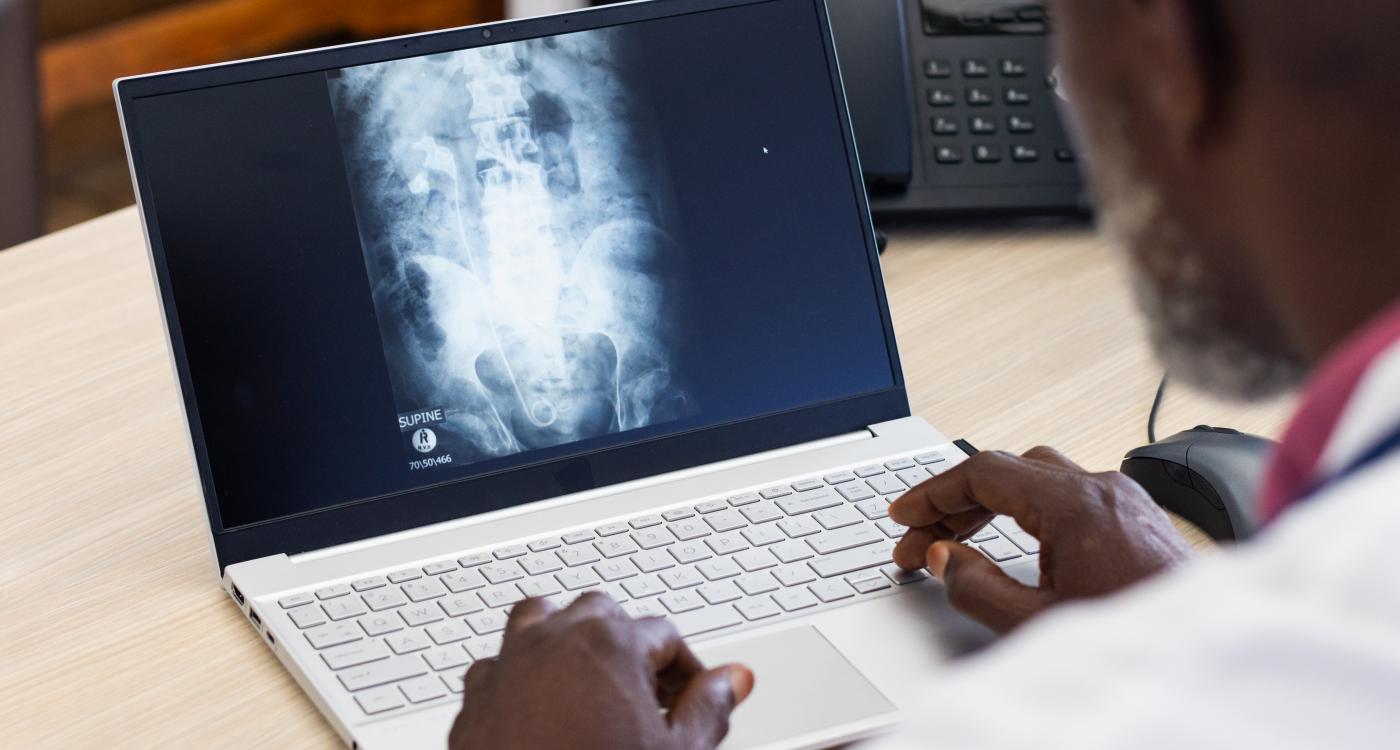
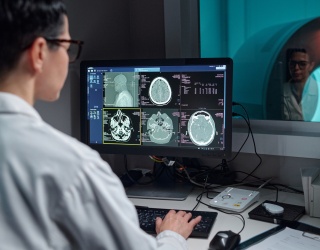
At RSNA 2025, an international panel explored how remote radiology is influencing patients, radiologists, and healthcare systems. Moderated by Jay R. Parikh, Professor of Diagnostic Radiology at MD Anderson Cancer Center, the session brought together perspectives from Asia, Canada, and Australia to examine both the benefits and risks of an increasingly distributed imaging workforce.The topic remains pressing and a point of discussion when it comes to integrating remote radiology into existing workflows.
Remote radiology is no longer niche. According to workforce data cited during the session, 82% of radiology practices in the U.S. now allow some form of telework, and the global teleradiology market is projected to grow from $15.6 billion in 2024 to $60.3 billion by 2030.
Against this background, speakers addressed the discussion around three key questions: What does remote radiology mean for patients, radiologists, and healthcare systems?

What Remote Radiology Means for Patients
Dr. Niketa Chotai, breast radiologist and lead consultant radiologist at Radlink Imaging Center in Singapore, emphasized that remote radiology is primarily driven by access and timeliness. “Some emergency studies, including trauma, stroke, cannot wait. The golden hours are important for patient's outcome and also for the patient's overall prognosis,” she said.
One of the most immediate benefits is faster reporting. Citing international data, Chotai noted that turnaround times can drop from 43 hours to just four hours, significantly improving both emergency and routine workflows.
Remote radiology also addresses global disparities in access to imaging expertise. “There are about 85 radiologists per million population in high-income countries compared to just less than two in low-income countries,” she explained, highlighting the uneven distribution of services. Remote services can help bridge this gap by connecting patients with specialists across borders.
Subspecialization is another key advantage. Remote reporting allows cases to be routed to experts, improving diagnostic accuracy and patient management. “Patients may not need to travel physically to places to get their reporting done, waiting time is less, [...].”
At the same time, Chotai pointed to important limitations, particularly gaps in clinical information: “There is not enough available data regarding the patient about their prior studies or the clinical data, and that does hamper our radiology reporting quality, and this in turn is going to affect the patient,” Chotai said.
Communication gaps are another concern. “Poor communication leads to almost 20 percent of the patient safety incidents,” she noted, emphasizing the need for structured communication workflows. Technical constraints, regulatory concerns and data privacy, and cross-border data protection issues can further affect diagnostic quality and patient trust.
What Remote Radiology Means for Radiologists
For radiologists, remote work offers significant advantages. Dr. Jean M. Seely, professor in the Department of Radiology at the University of Ottawa and head of the breast imaging section, described how remote radiology has transformed breast imaging services in Canada, where vast distances and sparse populations make on-site coverage difficult.
For radiologists, the benefits include:
- Reduced commute time
- Improved work-life balance
- Lower burnout risk
- Greater flexibility
- Enhanced recruitment and retention
Operationally, remote reading can also enhance productivity. Seely noted that from a practice point of view it can help to improve the focus, reduce interruptions, thus beeing very helpful for high volume screening,”.
However, these advantages come with clinical trade-offs. The inability to perform physical examinations is a key limitation: “We have a loss of on-site clinical assessment we're not able to perform a palpation or correlate the symptoms,” she explained, highlighting the loss of direct clinical assessment.
Interaction with technologists and colleagues may also be affected. “Communication can be fragmented,” and there can be a loss of opportunity for consultation when radiologists are no longer working in shared reading environments. Medical-legal considerations are another concern, as remote workflows may increase the risk of interpretation errors, particularly when communication gaps or incomplete clinical information are involved.
What Remote Radiology Means for Healthcare Systems
From a leadership perspective, remote radiology enables scalability and operational flexibility. Imaging demand continues to rise due to technological advances, aging populations, and increasing clinical reliance on imaging. External teleradiology providers can expand reporting capacity and improve turnaround times, particularly for after-hours coverage and remote locations.
Dr. John P. Slavotinek, president of the Royal Australian and New Zealand College of Radiologists, noted: “You have scalability, growth in reporting capacity, ability, particularly if there's a time zone separation, to improve your after hours and subspecialty coverage.”
However, these benefits must be balanced against long-term considerations: “Clinician interaction is diminished,” Slavotinek warned, highlighting potential impacts on communication and clinical integration.
He also highlighted broader strategic concerns, including the potential commoditization of radiology. As reporting becomes more distributed, “people start to devalue the non-reporting aspects of our tasks, delivering MDTs, discussing with referrers, research, teaching, and other such factors." Financial and operational factors also play a role, including IT integration, regulatory compliance, and ongoing costs associated with external providers.
Hybrid Models as the Emerging Standard
Across all perspectives, a consistent conclusion emerged: fully remote radiology has limitations, but a hybrid approach can capture most benefits while mitigating risks. “A hybrid model offers the best of both worlds,” Slavotinek said, while emphasizing the need to consider long-term strategic implications.
By combining on-site presence for procedures, multidisciplinary collaboration, and training with remote reporting, hybrid workflows can improve efficiency while maintaining quality and communication. Artificial intelligence is expected to further support remote radiology by triaging cases, improving workflow efficiency, and supporting diagnostic accuracy, although it introduces additional governance considerations.
A structural shift in Imaging
Panelists agreed that remote radiology is no longer a temporary response to workforce shortages or the COVID-19 pandemic. Instead, it represents a structural shift in how imaging services are delivered globally. By improving access to expertise, reducing geographic barriers, and offering flexible working conditions, remote radiology can strengthen healthcare systems.
As Chotai concluded, “remote radiology has come a long way and it has become such an important part that I don't think any one of us can now see radiology services without remote reporting.” It will remain integral to future practice, but gaps in clinical information and communication must be addressed to maintain trust and quality of care.